Chapter 6: Lumbar Spine
Objectives:
- Describe the anatomy of the lumbar spine including articulations, muscular and ligamentous attachments, and planes of motion
- Palpate and diagnose somatic dysfunction in the lumbar spine and be able to interpret a diagnosis based on landmark findings
- List the major muscles and actions of the muscles attached to the lumbar spine that are responsible for its motion, including flexion, extension, sidebending and rotation
- Demonstrate the appropriate setup and execution of lumbar muscle energy and HVLA for type 1 or type 2 lumbar somatic dysfunction
- Identify and locate the anterior and posterior lumbar counterstrain points
Anatomy and Musculature of the Lumbar Spine
Similar to the thoracic spine, the three main functions of the lumbar spine are to protect the spinal cord, to allow movement, and to support the upper body. As the transition from the thoracic spine to the lumbar spine occurs, the curvature changes from kyphosis in the thoracic spine to lordosis in the lumbar spine. The lumbar spine is a frequent site of pain, strain, and disability. Facet joints are oriented backward, upward, and medial.
At the level of L2, the spinal cord becomes the conus medullaris and the remaining nerves from L3-S5 exit from their respective nerve roots. From L2-L5, the spine is a collection of nerve roots that are freely floating. The dura mater continues down to the S2 level to the level of S5, beyond the conus medullaris.
Analogous anatomic structures in the thoracic spine which are found in the lumbar spine were introduced and defined in Chapter 4. The intervertebral discs of the lumbar spine are the largest of all the vertebrae to provide its weight-bearing function. There are two intervertebral foramen formed by 2 adjacent vertebral bodies and discs; 2 adjacent pedicles, an inferior articular process of a vertebra and the superior articular process of the next, form the intervertebral foramen. The intervertebral disc is made up of the annulus fibrosis (contains nociceptive/pain-sensing fibers) and the nucleus pulposus (shock absorption).
The ligaments, similarly, to the thoracic spine, include, posteriorly, the supraspinous ligament, the intertransverse ligament, the ligamentum flava, and the capsular ligament; anteriorly, include the anterior longitudinal ligament and the posterior longitudinal ligament; other ligaments include the iliolumbar ligament. The anterior longitudinal ligament provides stability to the anterior portion of the vertebral column and prevents hyperextension; it is very broad and spans almost the entire width of the vertebral body. The ligamenta flava forms the posterior portion of the spinal cord canal. The posterior longitudinal ligament forms the anterior wall of the spinal canal and prevents excessive flexion; compared to the anterior longitudinal ligament it is thinner by comparison. The intertransverse ligament spans the entire length of the vertebral body and the anterior/posterior portions.
Key muscles of the lumbar spine are listed in Table 6.1 and include the respiratory diaphragm, latissimus dorsi (which connects the lumbar spine to the upper extremities), erector spinae muscles (longissimus thoracis, spinalis thoracis, and multifidus), and the core muscles. Additional important muscles include interspinalis muscles and the intertransversarii muscles. The intertransversarii muscles, when unilaterally contracted, will produce isolated sidebending of the lumbar spine. The core muscles stabilize the spine and posture.
| Origin | Insertion | Action | Innervation | Schematic (from Thieme) | |
|---|---|---|---|---|---|
| Respiratory diaphragm: |
|
Central tendon | Respiration | Phrenic nerve (C3-C5) | 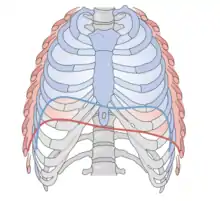 Diaphragm: red - inhalation; blue - exhalation |
| Psoas (psoas major; part of Iliopsoas) | T12-L4 vertebral bodies | Lesser trochanter of the femur |
|
Femoral nerve and lumbar plexus | 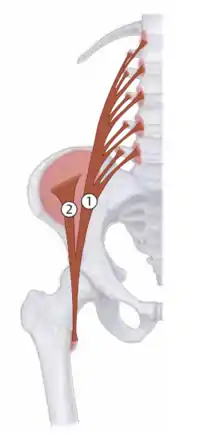 Iliopsoas: 1 - Psoas major |
| Latissimus dorsi |
|
Lesser tuberosity of the humerus |
|
Thoracodorsal nerve (C6-C8) | 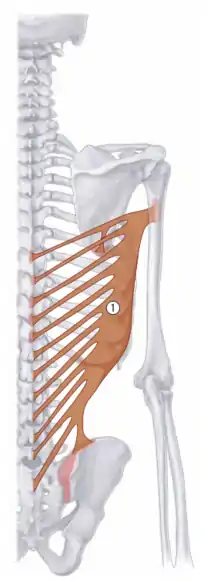 1 - Latissimus dorsi |
The lumbar spine is rife with potential pathology. Zygapophyseal tropism is the most common anomaly in the lumbar spine where there is asymmetry of the bilateral facet joints. Spina bifida has three variants: (1) spina bifida occulta (malformation of the vertebrae with no overt sign/symptoms except for a tuft of hair over the affected vertebrae), (2) spina bifida with meningocele (where the meninges protrude into a space created by the malformation and can be repaired with surgery with minimal residual nerve damage), and (3) spina bifida with meningomyelocele (where the spinal cord herniates into the fluid-filled space leading to incontinence, ambulatory dysfunction, and other problems).
Nerve roots in the lumbar spine exit the intervertebral foramen below the corresponding vertebrae. (Analogous to the thoracic spine.) Radiculopathy is pain that follows the distribution of the involved nerve root. Paresthesias (best describes as “pins and needles” or “numbness and tingling”) occurs in a dermatomal pattern.
Lumbar disc herniations occur most commonly due to a narrowed posterior longitudinal ligament leading to herniation of the nucleus pulposus in the posterolateral direction. Almost all of the lumbar disc herniations seen on imaging (typically MRI) occur between L4-L5 or L5-S1. Decreased or absent patellar reflexes with decreased sensation on the medial aspect of the ankle, weakness of ankle dorsiflexion, and weakness on knee extension are symptoms of a herniated nucleus pulposus. The straight leg raise test is done to assess for disc herniation. The patient lays supine and the physician passively flexes the hip while the knee is in full extension. The test is considered positive if pain is elicited. Additionally, dorsiflexion of the foot can be added at the end of passive flexion to assess for the presence of disc herniation in the L4-S1 nerve roots.
Spondylosis is degenerative changes within the intervertebral disc and ankylosing of adjacent vertebral bodies. On X-ray, this appears as anterior lipping of the vertebral bodies. Spondylolysis (not to be confused with spondylosis) occurs as a defect of the pars interarticularis without anterior displacement of the vertebrae. This is best seen on oblique X-rays and has the characteristic appearance of a “collar on the neck of a Scottie dog”. Spondylolisthesis occurs as a defect of the pars interarticularis with anterior displacement of one vertebra on the vertebra below. This is diagnosed with lateral X-rays, and especially oblique series.
Meralgia paresthetica is a condition characterized by paresthesias in the outer part of the thigh and is caused by compression of the lateral femoral cutaneous nerve, which supplies sensation to the upper leg.
Psoas syndrome is characterized by pain or injury to the psoas muscle. (See Table 6.1.) The Thomas test assesses the presence of a flexion contracture of the hip. The patient lays supine and the physician flexes the knee to the patient’s abdomen. The test is positive if the opposite leg lifts off the table and negative if the leg remains flat on the table.
It is critically important to assess low back pain for more emergent pathology. For example, a history should inquire about recent trauma; progressive weakness; new-onset low back pain associated with weight loss, fever, and lymphadenopathy is concerning for bone metastasis; recent infection; IV drug abuse; ruling out cauda equina syndrome. Cauda equina syndrome is a neurosurgical emergency characterized by lower extremity paresthesias (numbness/tingling), saddle anesthesia, and fecal and urinary incontinence and requires immediate intervention. Other chronic pathology should also be considered such as osteoporosis, whether secondary to chronic corticosteroid use or advanced age; morning stiffness, alternating buttocks pain, or awakening due to back pain in the night; back pain with leg pain in the L4, L5, and S1 sensory distribution; and radiating leg pain of an older patient with symptoms lasting greater than one month.
Somatic Dysfunction of the Lumbar Spine
The main motion of the lumbar spine is flexion and extension; sidebending and rotation are also motions associated with the lumbar spine. Like the thoracic spine, the lumbar spine follows Fryette’s Laws of Physiologic Motion.
Though this will be discussed in more detail in Chapter 7 (Pelvis, Sacrum, and Innominates), mechanics of the lumbosacral spine demonstrate that sidebending of L5 will cause the sacrum to rotate on a sacral oblique axis on the same side and rotation of L5 will cause the sacrum to rotate on a sacral oblique to the opposite side. Using relevant landmarks such as the iliac crest (at the level of L4), sacral base (at the level of S1), or bottom of the ribcage (at the level of T12) will help to correlate palpatory findings with vertebral levels. By asking a patient to assume a Sphinx position, an extension dysfunction can be diagnosed if the transverse prominence improves.
Fryette’s Laws of Physiologic Motion dictate biomechanics of somatic dysfunction of the thoracic and lumbar spine:
- Fryette’s First Law states when the thoracic and lumbar spine are in a neutral position, the coupled motion of sidebending and rotation for a group of vertebrae occur to opposite sides.
- Fryette’s Second Law states when the thoracic and lumbar spine is sufficiently flexed or extended (non-neutral), the coupled motions of sidebending and rotation in a single vertebra occur to the same side; the facet joints are engaged and dictate which direction the body of the vertebrae moves.
- Fryette’s Third Law states initiating motion of a vertebral segment in any plane of motion will modify the movement of that segment in other planes of motion
| Example: Somatic dysfunction nomenclature |
|---|
Type 1 dysfunction:
(in type 1 dysfunctions, sidebending is written first) |
Type 2 dysfunction:
(in type 2 dysfunctions, rotation is written first) |
With right sidebending, the right transverse process moves inferiorly, the left transverse process moves superiorly, and a concavity is noted on the sidebent side. (Likewise, convexity is noted on the contralateral side.)
| Example: Diagnosing lumbar spine somatic dysfunctions |
|---|
| Upon palpation of a patient’s lumbar spine, L3 is found to have a prominent transverse process on the right. The L3 location is verified by locating the iliac crest and moving up one vertebral level. The transverse processes of the vertebrae above and below this level are unremarkable. With extension, the prominence of the transverse process of L3 is not appreciated. With flexion, the prominence is more apparent. The somatic dysfunction diagnosis is L3 ERRSR. |
Treatment of Somatic Dysfunction of the Lumbar Spine
Myofascial release techniques:
| Thoracodorsal fascia: The patient is prone. Place both hands on opposite sides of the thoracodorsal fascia. Apply enough pressure to engage the fascial tissue until sufficient end feel is reached. Assess motion of the tissue in all 3 planes of motion: anterior/posterior (representing flexion and extension), clockwise and counterclockwise twisting (representing rotational component), and tilting from one hand to the other (representing the sidebending component). Ease of motion in all planes is determined. This technique can then be used as either a direct or an indirect technique. If performing a direct technique, bring the fascia into patient’s barrier in all three planes of motion. If performing an indirect technique, bring the fascia in all three planes into its ease of motion. Hold the tissues in either the ease or barrier of motion in all three planes. This force is held for approximately 30-60 seconds or until a release is palpated. | 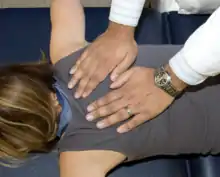 Thoracodorsal Fascia Myofascial Release |
Post-isometric muscle energy techniques:
| Type 1 dysfunction (seated): The patient is seated on the table, while the physician stands behind the patient. One hand monitors the transverse process of the vertebrae at the apex of the curve on the rotational side (left side if the group is rotated to the left, right side if the group is rotated to the right). The other hand is placed across the patient’s shoulders, it may be helpful to have the patient hold their elbows in a genie type position. The patient’s lumbar spine is kept in the neutral position, then using the shoulders for control, the spine is sidebent and rotated into its barriers of motion (sidebending occurs towards the convexity and rotation occurs away from the convexity). The patient is then instructed to sidebend and rotate their body toward their ease of motion (towards the diagnosis) and this force is met by the physician to produce an isometric contraction. | 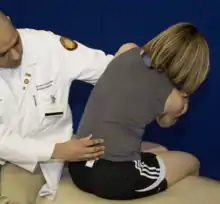 Type 1 Lumbar Somatic Dysfunction Seated |
| Type II dysfunction (seated): The patient is seated on the table, while the physician stands behind the patient. One hand monitors the transverse process of the vertebrae on the rotation side of the dysfunction. The other hand is placed across the patient’s shoulders, it may be helpful to have the patient hold their elbows in a genie type position. The patient’s lumbar spine is then flexed or extended into the barrier of motion, then using the body, the spine is sidebent and rotated into its barriers of motion. The patient is then instructed to sidebend or rotate their body toward their ease of motion (toward the diagnosis) and this force is met by the physician to produce an isometric contraction. | 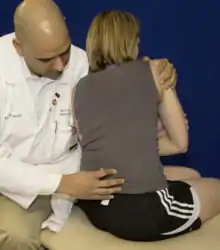 Type 2 Lumbar Somatic Dysfunction Seated |
| Lateral Recumbent: The patient is in recumbent position on the table, while the physician stands to the side of the table in front of the patient. While monitoring the desired segment, flex the hips and knees until motion is felt at the appropriate lumbar level. Maintaining the angle of hip flexion in the top lower extremity, ask the patient to straighten the bottom lower extremity to neutral position. Secure the top lower extremity either by tucking the foot into the popliteal fossa of the bottom lower extremity, or by allowing the top lower extremity to hang off the table. While monitoring the desired segment, rotate the patient’s torso in the opposite direction of the lower extremities until motion is felt at the appropriate lumbar level. While maintaining the lockout on the desired segment, rotate the torso and top lower extremity in opposite directions until the restrictive barrier is reached. Ask the patient to rotate their pelvis posteriorly, and resist this force to create an isometric contraction. |  Lateral Recumbent Lumbar Muscle Energy |
HVLA techniques:
| The patient is in recumbent position on the table with the rotational side of the dysfunction down, while the physician stands to the side of the table in front of the patient. While monitoring the desired segment, flex the hips and knees until motion is felt at the appropriate lumbar level. Maintaining the angle of hip flexion in the top lower extremity, ask the patient to straighten the bottom lower extremity to neutral position. Secure the top lower extremity either by tucking the foot into the popliteal fossa of the bottom lower extremity. While monitoring the desired segment, rotate the patient’s torso in the opposite direction of the lower extremities until motion is felt at the appropriate lumbar level. While maintaining the lockout on the desired segment, rotate the torso and top lower extremity in opposite directions until the restrictive barrier is reached. Keeping physician center of gravity posterior to the patient’s greater trochanter, provide a high velocity, low amplitude vertical thrust through the patient’s upper innominate. For a type 1 dysfunction, rotate the torso and top lower extremity in opposite directions (i.e. pulled apart) until the restrictive barrier is reached before applying a thrust; for a type 2 dysfunction, they are rotated toward each other (i.e. brought together). |  Lumbar Roll HVLA |
| Lumbar counterstrain tenderpoints |
|---|
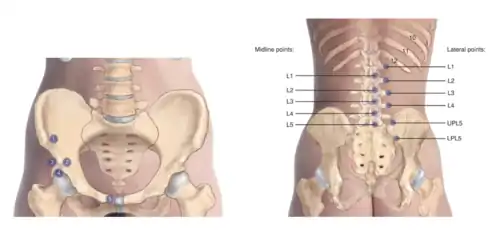 Lumbar Counterstrain Tenderpoints |
Reference: 1. Nicholas AS, Nicholas EA. Atlas of Osteopathic Techniques. Philadelphia, PA: Lippincott Williams and Wilkins, 2016. Pages 185 and 195.
| Tenderpoint | Location | Treatment position (initial setup) |
|---|---|---|
| AL1 | Medial to ASIS | Supine with hip/knee flexion |
| AL2 | Medial to AIIS (AIIS = anterior inferior iliac spine) |
|
| AL3 | Lateral to AIIS |
|
| AL4 | Inferior to AIIS |
|
| AL5 | Anterior aspect of pubic bone 1 cm lateral to pubic symphysis just inferior to prominence |
|
| Tenderpoint | Location | Treatment position (initial setup) |
|---|---|---|
| PL1-PL5 | Inferolateral aspect of spinous process or laterally on transverse process of dysfunctional segment | Patient prone with hip E SARA |
| PL3 lateral gluteus (iliac crest) | Halfway between UPL5 and PL4 at inferior aspect of posterior iliac crest near gluteus medius/maximus | Patient prone; E ER Add |
| PL4 lateral gluteus (iliac cest) | Posterolateral pelvic edge halfway between greater trochanter and iliac crest at gluteus maximus | Patient prone; E ER Add |
| UPL5 (upper pole) | Superior surface of PSIS | Patient prone with hip extension; E ER Add |
| LPL5 (lower pole) | 2 cm below PSIS on the ilium | Patient prone with hip flexed off the table and with slight adduction; F IR Add |
Review questions
Questions 1-5: Identify the location of the tenderpoints on the anterior lumbar spine.
1. AL1
2. AL2
3. AL3
4. AL4
5. AL5
A. Inferior to the AIIS
B. Medial to the AIIS
C. Lateral to the AIIS
D. Medial to the ASIS
E. 1 cm lateral to the pubic symphysis
6. A patient presents for evaluation of low back pain. She has tenderness to palpation of the left lumbar spine, hypertonic lumbar paraspinal muscles, decreased lumbar extension, and a prominent transverse process of L2 on the right. Muscle strength testing, deep tendon reflexes, and sensation testing are unremarkable. What would the initial setup be for a seated muscle energy technique for the treatment of this somatic dysfunction?
A. Torso extended, rotated left, sidebent right
B. Torso extended, rotated left, sidebent left
C. Torso flexed, rotated right, sidebent right
D. Torso extended, rotated right, sidebent left
E. Torso flexed, rotated right, sidebent left
F. Torso flexed, rotated left, sidebent left
7. A patient presents for evaluation of low back pain. She has tenderness to palpation of the left lumbar spine, hypertonic lumbar paraspinal muscles, decreased lumbar extension, and a prominent transverse process of L2 on the right. Muscle strength testing, deep tendon reflexes, and sensation testing are unremarkable. Where should the vector of force be directed for lateral recumbent HVLA for the treatment of this somatic dysfunction?
A. Downward into the table with the cephalad hand and slightly posterior into the shoulder with the caudad hand
B. Superior with the caudad hand and inferior with the cephalad hand
C. Inferior with the caudad hand and superior with the cephalad hand
D. Downward into the table with the caudad hand and slightly posterior into the shoulder with the cephalad hand
8. Where does the nerve root for L3 exit the intervertebral foramen?
A. Between L1 and L2
B. At the level of L2
C. Between L2 and L3
D. At the level of L3
E. Between L3 and L4
9. Which of the following is true regarding motion of the lumbar spine?
A. The main motion of the lumbar spine is rotation
B. Motion of the lumbar spine does not follow Fryette's Laws of Physiologic Motion
C. The alignment of the super facet joint is backward, downward, and lateral
D. The rotation of L5 will cause the sacrum to rotate to the same side.
E. The rotation of L5 will cause the sacrum to rotate to the opposite side.
10. A patient is noted to have a right foot drop. What spinal nerve roots are affecting this observation?
A. T5-T9
B. T10-T11
C. T12-L2
D. L5-S1
E. S2-S4
11. What is the most common direction of a herniated nucleus pulposus?
A. Anteromedial
B. Anterolateral
C. Posteromedial
D. Posterolateral
E. Anterior
F. Posterior
12. Which of the following is not a “red flag” cause for low back pain?
A. Pain at night
B. Unexplained weight loss
C. Bowel or bladder incontinence
D. Sexual dysfunction
E. Unilateral dull achy pain
Answers to Review Questions
- D
- B
- C
- A
- E
- B
- D
- E
- E
- D
- D
- E