Chapter 3: Cervical Spine
Objectives:
- Identify the major muscles associated with cervical spine motion
- Define segmental rotation restriction
- Introduce clinical significance of cervical spine somatic dysfunction
Anatomy and Musculature of the Cervical Spine
As we begin our survey of the axial skeleton, a discussion of the foundation of the musculature and anatomy of each system is necessary. When learning muscles, knowing the origin and insertion is key to understanding the action – that is, how does the muscle shorten? In general, muscles that originate or insert on the anterior surface of the body are flexors. Likewise, those that originate or insert on the posterior surface of the body are extensors. (Table 3.1)
The direction in which a muscle shortens dictates its action. For example:
- Anteriorly-located muscles are typically flexors
- Posteriorly-located muscles are typically extensors
- Laterally-located muscles are typically lateral flexors (or sidewinders)
- Muscles that span over two or more surfaces will have several actions determined by how the muscle shortens
| Flexors | Extensors | Rotators | Sidebenders |
|---|---|---|---|
|
|
|
|
Two muscles worth mentioning specifically are the sternocleidomastoid muscle and the scalene muscles because of their importance in cervical spine biomechanics. Torticollis is a dysfunction of the sternocleidomastoid muscle in which the muscle is hypertonic, resulting in a “tilted neck” appearance. A right-sided torticollis will have a hypertonic right sternocleidomastoid muscle where the cervical spine appears sidebent to the right and rotated to the left (SRRL) as a result of the muscle action.
| Origin | Insertion | Action | Innervation | Schematic (from Thieme) | |
|---|---|---|---|---|---|
| Sternocleidomastoid |
|
Mastoid process and superior nuchal line |
|
CN XI and C1-C2 branches of the cervical plexus | 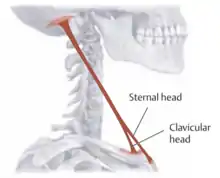 Sternocleidomastoid |
| Scalene muscles (anterior, middle, and posterior): |
|
|
|
Cervical plexus and brachial plexus (C3-C6) |  Scalenes: 1 - anterior scalene; 2 - middle scalene; 3 - posterior scalene |
| Longus capitis | Anterior tubercle of C3-C6 vertebrae | Base of occiput |
|
Cervical plexus (C1-C4) | 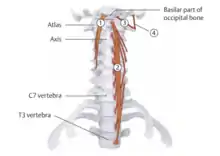 1 - longus capitis |
| Longus colli |
|
|
|
Cervical plexus (C2-C6) |  2 - longus colli |
| Rectus capitis anterior | Lateral mass of the atlas | Base of occiput |
|
C1 nerve |  3 - rectus capitis anterior |
| Rectus capitis lateralis | Transverse process of the atlas | Base of occiput |
|
C1 nerve |  4 - rectus capitis lateralis |
The three muscles that comprise the suboccipital triangle and their respective locations are:
- Rectus capitis posterior major – above and medially
- Obliquus capitis superior – above and laterally
- Obliquus capitis inferior – below and laterally
| Origin | Insertion | Action | Innervation | Schematic (from Thieme) | |
|---|---|---|---|---|---|
| Rectus capitis posterior major | Spinous process of the axis (C2) | Inferior nuchal line of the occipital bone |
|
Dorsal ramus of C1 | 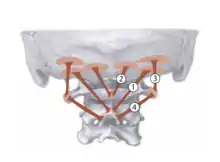 1 - rectus capitis posterior major |
| Obliquus capitis superior | Lateral mass of the atlas | Lateral half of the inferior nuchal line |
|
Suboccipital nerve |  3 - obliquus capitis superior |
| Obliquus capitis inferior | Spinous process of the axis | Lateral mass of the atlas | Rotation of the head and neck | Suboccipital nerve |  4 - obliquus capitis inferior |
Somatic Dysfunctions of the Cervical Spine
Important skeletal components of the cervical spine include for the vertebrae: the transverse process, spinous process, vertebral arch, lamina, pedicle, body, transverse foramen, posterior tubercle, anterior tubercle, superior articular process, and inferior articular process of each level of the vertebrae. C1 and C2 are considered atypical. C1 lacks both a spinous process and a vertebral body. C2 has a dens that projects superiorly and articulates with C1. C2-C6 have bifid (i.e. split into two) spinous processes. The articular pillars are located posterior to the transverse processes and are used for diagnosing somatic dysfunctions. The nerves which exit the cervical spine at the level of C3, C4, and C5 come together to form the phrenic nerves (present bilaterally) which innervate the respiratory diaphragm. There are eight nerves which exit above the spinal level of the corresponding cervical vertebrae; C8 exits above T1.
The regions of the cervical spine can be classified as atypical cervical vertebrae, made up of the occipitoatlantal joint (the OA joint) and the atlantoaxial joint (the AA joint), and the typical cervical vertebrae, which include the bottom of C2 to C7. The occipitoatlantal joint (also known as C0 on C1) dictates its motion: 50% of the flexion and extension of the cervical spine occurs at the OA joint. Sidebending and rotation occur in opposite directions. This can be represented in nomenclature as OA SXRY, where X and Y represent opposite directions. Movement of the occipitoatlantal joint occurs in the sagittal plane (i.e. in flexion and extension). In a flexion somatic dysfunction, the condyles have moved posterior in relation to C1, the space between the occiput and C1 feels deeper, and the patient looks like their chin is tucked. In an extension somatic dysfunction, the condyles move anterior in relation to C1, the space between the occiput and C1 feels shallower, and the patient looks like their chin is sticking out. The patient can be assessed by looking for deviation of the chin and the tip of the nose from the mid-line position. The atlantoaxial joint (the AA joint, also known as C1 on C2) dictates its motion: 50% of rotation of the cervical spine occurs at the AA joint. The AA joint is an example of a saddle joint. There is no sidebending component to AA motion; all of the motion is rotation about a vertical axis. Somatic dysfunctions occur in left and right rotation at the AA joint. Upon inspection, the head may be deviated to the left or the right. Palpation of the traverse process of the atlas may feel posterior (closer to the mastoid process) on the side of the rotation. When performing motion testing, there will be a preference for rotation in one direction and a limitation in the opposite direction.
| Example: OA somatic dysfunction |
|---|
| If a patient has a difficulty moving posteriorly in the sagittal plane, has difficulty sidebending to the left, and rotating to the right, the diagnosis would be OA FSRRL. Motion occurs in the sagittal (flexion/extension), coronal (sidebending), and transverse (rotation) planes, respectively, with this dysfunction. |
The typical cervical vertebrae superior facet joint orientation is backward, upward, and medial. Physiologic motion of the cervical spine is determined by the facet joint orientation. Flexion and extension somatic dysfunctions of typical cervical vertebrae are identified in Table 3.2. In the typical cervical vertebrae, sidebending and rotation occur to the same side. In the neutral position, sidebending precedes rotation (i.e. SXRX). In flexion or extension, rotation precedes sidebending (i.e. RXSX).
| Flexion somatic dysfunction: | Extension somatic dysfunction: |
|---|---|
|
|
To summarize cervical spine motion (Table 3.3):
| Level | Major motion | Diagnosis |
|---|---|---|
| OA | Flexion and Extension (50%) | (F) or (E); SXRY |
| AA | Rotation only | RL or RR |
| C2-C7 | Sidebending and rotation; Flexion and extension | Neutral or (F)/(E); RXSX |
The anatomy and biomechanics of the cervical spine result in the following possible somatic dysfunctions (and nomenclature examples):
- OA flexion dysfunction: sidebending/rotation to opposite sites (OA FSXRY)
- OA extension dysfunction: sidebending/rotation to opposite sides (OA ESXRY)
- AA restriction of rotation (AA RX)
- C2-C7 flexion dysfunction: sidebending/rotation to the same sides (C2 FRXSX)
- C2-C7 extension dysfunction: sidebending/rotation to the same sides (C2 ERXSX)
- C2-C7 neutral dysfunction: sidebending/rotation to the same sides (C2 RXSX)
Structural diagnosis of the atypical cervical spine is done by introducing translation of the head from right to left while the OA is flexed or extended while sensing for resistance. Translation is a coupled movement involving sidebending to the opposite side and rotation to the same side. The AA is assessed by flexing the patient’s head and neck to a 45o angle to lock out the typical cervical segments. Assessing rotation to each side is done to determine restriction.
Structural diagnosis of the typical cervical spine requires palpation of the spinous processes (for flexion/extension) of the typical vertebrae and an appreciation of the articular pillars (for rotation), which are located 2-3 cm from the respective spinous process. The spinous process of C2 is the first bony prominence palpable below the inion. The spinous process of C7 (the vertebra prominens) remains palpable during cervical extension. With fingertips between C2 and C7, finger pads will fall on C3, C4, C5, and C6. Motion testing is achieved by contacting the articular pillar with the index finger bilaterally. Sidebending is assessed pushing inferomedially. Rotation can be assessed by rotating toward the opposite side. The transverse processes of the cervical spine are shorter and cannot be appreciated to the same extent as the articular pillars. The vertebral artery passes through the transverse processes of the cervical spine bilaterally.
| Example: Cervical somatic dysfunctions |
|---|
| If the head is translated from right to left while the OA is extended, and resistance is felt, motion restriction is backward bending, right sidebending, and left rotation. Therefore, the somatic dysfunction (and diagnosis) is OA FSLRR. If the AA joint is assessed and found to have restriction with right rotation, the somatic dysfunction (and diagnosis) is AA RL. If a physician diagnoses C4 FRLSL on a patient, the articular pillar on the right is slightly posterior and becomes more posterior in extension. |
Treatment of Somatic Dysfunction of the Cervical Spine
The cervical spine, as with the rest of the axial spine and the upper and lower extremities may be treated by utilizing soft tissue/myofascial release, muscle energy, HVLA, counterstrain, and other techniques. After performing a technique, the patient should be reassessed in the same manner in which they were initially assessed and diagnosed.
Myofascial release/Soft tissue techniques of the cervical spine:
|
Longitudinal stretch: Patient is supine and physician is sitting at the head of the patient. Palpate the paraspinal musculature of the cervical spine bilaterally and using alternating movements, apply a deep palpation to the musculature working distally to proximally in a figure eight fashion. Please be sure that there is adequate pressure to engage the muscle fibers and not only the skin. Repeat until the fibers begin to loosen. |
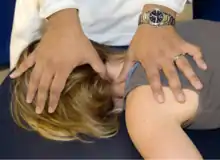 Cervical soft tissue longitudinal stretch |
|
Perpendicular stretch (90 degrees to the cervical muscle fibers): Patient is supine and physician stands to one side of the patient. Apply deep palpation to the musculature and pull laterally until barrier is reached. Be sure to stabilize the patient’s head to prevent it from rotating. Continue with same technique on different section of cervical muscle fibers, repeating as necessary until the fibers begin to loosen. |
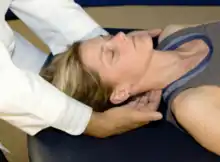 Cervical soft tissue perpendicular stretch |
|
Suboccipital release: Patient is supine on the treatment table. Place fingertips at the base of the occiput, letting the weight of the head hang on the fingertips. Wait for the musculature that attaches at the base of the occiput to relax or release. |
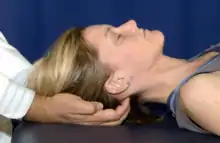 Cervical soft tissue suboccipital release |
|
OA decompression: Place the patient supine on the treatment table. Place fingertips at the base of the occiput (at about a 45 degree angle) and applies a cephalad traction, that is held for a few seconds until a loosening or increase in ease of motion is appreciated. |
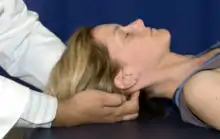 Cervical soft tissue OA decompression |
|
Myofascial release: Patient can be in any position. Palpate the desired layer fascia by exerting an appropriate amount of pressure onto the cervical spine Motion tests the fascia in all planes of motion: longitudinal, perpendicular and rotation. For a direct treatment, take the fascia into all planes of restriction and hold until a release is palpated. For an indirect treatment, take the fascia into all planes of ease and hold until a release is palpated. |
Muscle energy is a direct technique where the patient is placed into their barrier and the patient pushes away from that barrier. Restriction in any plane of motion can be used alone or in combination with other restrictions. To treat the cervical spine with a muscle energy technique, the patient is taken into the restrictive barrier and attempts to return to neutral while the physician resists with an isometric pressure. The process is completed 3-5 times for 3-5 seconds each, with a final stretch at the end of the treatment before re-assessing.
Muscle energy techniques of the cervical spine:
|
OA vertebral segment: Place the patient supine on the treatment table. Place the OA into the position of greatest restriction (i.e. opposite the diagnosis). Maintain this barrier and ask patient to return their head to neutral position. The isometric contraction occurs for 3-5 seconds, and is repeated for 3-5 cycles, resetting the OA to a new restrictive barrier after each successive contraction. Perform a final stretch after the final isometric contraction. |
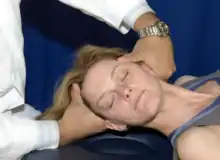 Cervical muscle energy of OA |
|
AA vertebral segment: Place the patient supine on the treatment table. Place the MCP joint of the index finger over the AA. While in neutral, bring the patient to their rotational barrier of the AA (45 degrees of flexion). Maintain that barrier and instruct the patient to rotate their head back neutral position. The isometric contraction occurs for 3-5 seconds, and is repeated for 3-5 cycles, resetting the cervical rotation to the new restrictive barrier after each successive contraction. Perform a final stretch after the final isometric contraction. |
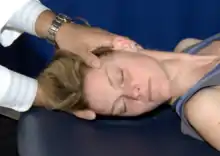 Cervical muscle energy of AA |
|
Typical cervical vertebrae: The patient is supine on the treatment table. Contact either the transverse process or the articular pillar of the dysfunctional segment with the MCP of the index finger on the same side as the rotation/sidebending dysfunction (i.e. for sidebent/rotated right, use right hand for contact). Sidebend the patient’s head towards the contact point until a sidebending barrier is engaged. Rotate the head in the opposite direction of the dysfunction until a rotational barrier is reached. Maintain that barrier and instruct the patient to rotate their head back to neutral position. The isometric contraction occurs for 3-5 seonds, and is repeated for 3-5 cycles, resetting the cervical rotation to the new restrictive barrier after each successive contraction. Perform a final stretch after the final isometric contraction. |
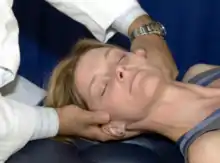 Cervical muscle energy of typical vertebrae |
HVLA technique setup is often the same position as the rotation restriction. HVLA techniques should be preceded with myofascial release techniques. Despite that HVLA is a direct technique, the setup is counterintuitive in that the patient is sidebent toward the side of the dysfunction and rotated away from the prominent articular pillar. It is critically important that the physician be in control of the patient’s head at all times and that the physician is comfortable when performing the technique by adjusting the table height and by repositioning to ensure maximum comfort. If a patient is unable to tolerate an HVLA technique, return to the neutral position and utilize another treatment model. Be alert for guarding, where a patient will become tense just prior to the thrusting portion of the technique. Do not thrust on a guarding patient; this can lead to injury. HVLA is considered a safe technique, although rare complications have been reported.
HVLA techniques of the cervical spine:
|
Typical cervical vertebrae: The patient is supine on the treatment table. Contact the articular pillar of the dysfunctional segment with the MCP of the index finger on the same side as the rotation/sidebending dysfunction (i.e. for sidebent/rotated right, use right hand for contact). Sidebend the patient’s head towards the contact point until a sidebending barrier is engaged. Rotate the head in the opposite direction of the dysfunction until a rotational barrier is engaged. Maintain that barrier and without backing off apply a quick rotational thrust through the barrier. |
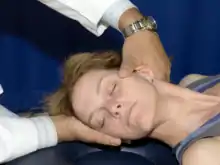 Cervical HVLA |
Counterstrain shortens the strained muscle by bringing the origin and insertion closer. A tenderpoint is a small area of soft tissue which is tender to touch. Tenderpoints can be located anteriorly and posteriorly. Counterstrain techniques are indirect techniques where the patient is taken into the position of ease, with some exceptions.
To perform a counterstrain technique:
- A tenderpoint is identified by inquiring to the patient about tenderness.
- The physician labels the tenderpoint as a 10/10.
- The muscle is positioned such that the tenderpoint is no longer painful. The physician flexes, extends, sidebends, and rotates the involved muscle or joint to a point where there is a 70% reduction in pain rating (i.e. the patient states “the pain is now a 3/10”).
- The tenderpoint is monitored with one finger while the area remains in the position of comfort for 90 seconds.
- The muscle/joint is slowly and passively returned to neural while the tenderpoint is continually monitored.
- The degree of tenderness at the tenderpoint is reassessed.
The tenderpoint locations and setups for the cervical spine are provided below. (Figure 3.1) Anterior tenderpoints are treated in flexion; posterior tenderpoints are treated in extension. Lateral tenderpoints require more sidebending and rotation components to the initial treatment setup.
| Cervical counterstrain tenderpoints |
|---|
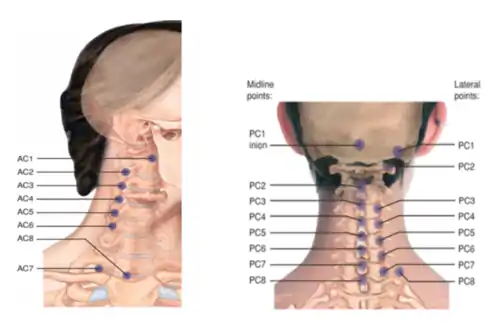 Cervical tenderpoints |
References:
- Nicholas AS, Nicholas EA. Atlas of Osteopathic Techniques. Philadelphia, PA: Lippincott Williams and Wilkins, 2016. Pages 156 and 161.
- Clay JH, Pounds DM. Basic Clinical Massage Therapy: Integrating Anatomy and Treatment. Baltimore, MD: Lippincott Williams and Wilkins, 2003.
- AC1 is RA (rotated away)
- AC7 is F STRA (sidebend toward, rotate away)
- Everything else is F SARA (sidebend away, rotate away)
- Anterior tenderpoints are located over the anterior surface of the transverse processes.
| Tenderpoint | Location | Treatment position (initial setup) | Acronym |
|---|---|---|---|
| AC1 mandible | On the posterior aspect of the ascending ramus of the mandible at the level of the earlobe | Rotate away with minimal flexion and sidebending away | RA |
| AC1 transverse process | On the lateral aspect of the C1 transverse process midway between the ramus of the mandible and the mastoid process | Rotate away with minimal flexion and sidebending away | RA |
| AC2-AC6 | On the anterior lateral aspect of the anterior/posterior tubercles of the transverse process of the corresponding cervical vertebrae | Flex to the level of the dysfunctional segment; sidebent away; rotate away | F SARA |
| AC7 | On the posterosuperior surface of the clavicle at the clavicular attachment of the sternocleidomastoid muscle | Flex to the level of C7; sidebend toward; rotate away | F ST RA |
| AC8 | On the superior medial end of the clavicle at the sternal attachment of the sternocleidomastoid muscle | Flexx, but less than AC7, sidebend away, rotate away | F SA RA |
- PC1 inion is F
- PC3 midline spinous process is F SARA
- Everything else is E SARA
- Lateral tenderpoints are located over the transverse processes; midline points are located over the spinous processes
| Tenderpoint | Location | Treatment position (initial setup) | Acronym |
|---|---|---|---|
| PC1 inion | On the inferior nuchal line lateral to the inion | Flexion of the occipitoatlantal joint; sidebend toward; rotate away | F |
| PC1 occiput | On the inferior nuchal line midway between the inion and the mastoid; associated with the suboccipital triangle musculature | Extension of the occipitoatlantal joint with mild compression of the head; sidebend away; rotate away | E SA RA |
| PC2 occiput | On the inferior nuchal line within the semispinalis capitis muscle | Extension of the occipitoatlantal joint with mild compression of the head; sidebend away; rotate away | E SA RA |
| PC2 midline spinous process | On the superior or superolateral tip of the spinous process of C2 | Extension of the occipitoatlantal joint with mild compression of the head; sidebend away; rotate away | E SA RA |
| PC3 midline spinous process | On the inferior or inferolateral aspect of the tip of the spinous process of C2 | Flex; sidebend away; rotate away | F SARA |
| PC4-PC8 midline spinous process | On the inferior or inferolateral aspect of the spinous process
|
Extend to the level of the dysfunctional segment; sidebend away; rotate away | E SARA |
| PC3-PC7 lateral | On the posterolateral aspect of the articular process associated with the respective dysfunctional segment | Extend to the level of the dysfunctional segment; sidebend away; rotate away | E SARA |
Some special considerations:
- The anterior tenderpoint for C1 is located behind the mandible near the transverse process of C2.
- The anterior tenderpoint for C7 is located on the lateral sternocleidomastoid muscle just superior to the clavicle. The position for treatment of this tenderpoint (AC7) is flexion, sidebending toward the tenderpoint, and rotating away from the tenderpoint.
- The medial posterior tenderpoint for C1 is located approximately 2 cm below the inion. It is treated by placing the head into flexion.
Review Questions
1. A patient presents with significantly hypertonic paraspinal muscles in the cervical spine on the left. Active and passive range of motion testing is limited by the hypertonicity. Segmental motion testing reveals restriction of C3-C5 when rotated to the right and ease of motion of C3-C5 with left sidebending. There is no improvement in the dysfunction noted with either flexion or extension. Muscle strength testing, deep tendon reflexes, and sensation testing are unremarkable. If this patient were to be treated with an indirect technique, what would the initial setup position be?
A. The neck is flexed, sidebent to the left, and rotated to the left.
B. The neck is extended, sidebent to the left, and rotated to the left.
C. The neck is flexed, sidebent to the right, and rotated to the right.
D. The neck is neutral, sidebent to the right, and rotated to the right.
E. The neck is neutral, sidebent to the left, and rotated to the left.
2. What is the curvature of the cervical spine in standing anatomic position?
A. Lordosis
B. Kyphosis
C. The cervical spine has features of both lordosis and kyphosis.
D. The curvature of the cervical spine cannot be adequately described by either lordosis or kyphosis.
E. There is no curvature to the cervical spine.
3. A patient presents complaining of neck pain with an unknown mechanism of injury. On evaluation of occipitoatlantal motion, the OA is found to translate easier to the right and the ease is more pronounced in extension. Muscle strength testing, deep tendon reflexes, and sensation testing are unremarkable. What is the diagnosis of this somatic dysfunction?
A. OA ESLRR
B. OA FSLRR
C. OA ESRRL
D. OA FSRRL
E. OA ESLRL
4. A patient presents complaining of neck pain following a car accident during which he sustained whiplash. With the neck angled to 45 degrees, atlantoaxial motion is assessed. He is noted to have difficulty rotating to the right. What is the diagnosis of this somatic dysfunction?
A. AA RR
B. AA RL
C. AA FRR
D. AA FRL
E. AA ERR
5. Motion at the OA joint occurs in the ____ plane for flexion and extension, ____ for sidebending, and ____ for rotation.
A. sagittal; transverse; coronal
B. coronal; transverse; sagittal
C. transverse; sagittal; coronal
D. coronal; sagittal; transverse
E. sagittal; coronal; transverse
6. A patient presents complaining of left-sided neck pain. On examination, C6 is found to be more difficult to rotate to the left. The dysfunction improves with flexion of the cervical spine. Muscle strength testing, deep tendon reflexes, and sensation testing are unremarkable. What is the diagnosis of this somatic dysfunction?
A. C6 FRRSR
B. C6 ERRSR
C. C6 FRLSL
D. C6 ERLSL
E. C6 FRRSL
7. Why are the articular pillars used for palpation of somatic dysfunction instead of the transverse processes?
A. The transverse processes of the cervical spine are more prominent than the articular pillars and inhibit palpation of minor motion loss.
B. The transverse processes of the cervical spine are shorter and cannot be appreciated to the same extent as the articular pillars.
C. The vertebral artery passes through the articular pillars of the cervical spine bilaterally.
D. The transverse processes are located 2-3 cm from the respective spinous process.
8. Which of the following is correct regarding the use of counterstrain for treatment somatic dysfunctions of the cervical spine?
A. The anterior tenderpoint for C2 is located behind the mandible near the transverse process of C2.
B. The medial posterior tenderpoint for C2 is located approximately 2 cm below the inion. It is treated by placing the head into flexion.
C. The anterior tenderpoint for C7 is located on the lateral sternocleidomastoid muscle just superior to the clavicle.
D. The majority of anterior tenderpoints are treated in extension with sidebending and rotation occurring away from the tenderpoint.
E. Lateral tenderpoints are located over the articular pillars.
9. Which of the following is true regarding the anatomy of the typical cervical spine?
A. The typical cervical vertebrae superior facet joint orientation is backward, upward, and lateral.
B. In the typical cervical vertebrae, sidebending and rotation occur to opposite sides.
C. In the neutral position, sidebending precedes rotation for the typical cervical spine.
D. In flexion or extension, rotation follows sidebending for the typical cervical spine.
10. Which of the following describes the proper initial setup for treatment of a somatic dysfunction of the cervical spine using HVLA?
A. The patient is sidebent toward the side of the dysfunction and rotated away from the prominent articular pillar.
B. The patient is sidebent toward the side of the dysfunction and rotated toward the prominent articular pillar.
C. The patient is sidebent away from the side of the dysfunction and rotated away from the prominent articular pillar.
D. The patient is sidebent away from the side of the dysfunction and rotated toward the prominent articular pillar.
11. Which muscle attaches to the transverse processes of C3-C6 and unilaterally contracts to sidebend the head to the same side of the cervical spine?
A. Splenius capitis
B. Longus colli
C. Anterior scalene
D. Trapezius
E. Sternocleidomastoid
12. Which of the following muscles does not comprise the subocciptal triangle nor have their location correctly designated?
A. Rectus capitis posterior minor – below and medially
B. Rectus capitis posterior major – above and medially
C. Obliquus capitis superior – above and laterally
D. Obliquus capitis inferior – below and laterally
Answer Key to Review Questions
- E
- A
- A
- B
- E
- A
- B
- C
- C
- A
- C
- A