Mycetoma
Mycetoma is a chronic infection in the skin caused by either bacteria (actinomycetoma) or fungi (eumycetoma), typically resulting in a triad of painless firm skin lumps, the formation of weeping sinuses, and a discharge that contains grains.[1] 80% occur in feet.[1]
| Mycetoma | |
|---|---|
| Specialty | Infectious diseases |
| Symptoms | Triad: painless firm skin lump, multiple weeping sinuses, grainy discharge[1] |
| Usual onset | Slowly progressive[1] |
| Types |
|
| Diagnostic method | Ultrasound, fine needle aspiration[1] |
Most eumycetoma is caused by M. mycetomatis, whereas most actinomycetoma is caused by N. brasiliensis, S. somaliensis, A. madurae and Actinomadura pelletieri.[1] People who develop mycetoma likely have a weakened immune system.[1] It can take between 3 months to 50 years from time of infection to first seeking healthcare advice.[1]
Diagnosis requires ultrasound and fine needle aspiration.[1]
While most cases of mycetoma occur in Sudan, Venezuela, Mexico, and India, its true prevalence and incidence are not well-known.[2][3] It appears most frequently in people living in rural areas, particularly in farmers and shepherds, who are often men between 20 and 40 years earning the primary incomes for their families.[1] It has been reported since 1840.[4] Noteworthy, the diagnosis of Mycetoma in non-endemic or low endemic areas as Europe and North Africa is challenging.[5][6] Physicians in these areas are usually unfamiliar with the disease-specific manifestations and need to exercise extra vigilance regarding those patients who are at high risk of contracting Mycetoma infections.[7] Recent evidence suggests that Egypt which borders Sub-Saharan Africa, is a low-endemic country.[5] Additionally, recent evidence suggests that Pakistan which borders India, is a moderate-endemic country.[8] Unlike bacterial acute hematogenous osteomyelitis and septic arthritis, misdiagnosed or delayed diagnosis of Mycetoma osteomyelitis can result in amputation or radical resection.[5] The disease is listed by the World Health Organization (WHO) as a neglected tropical disease.[3]
Risk
Frequent exposure to penetrating wounds by thorns or splinters is a risk factor.[9] This risk can be reduced by disinfecting wounds and wearing shoes.[10]
Pathogenesis
Mycetoma is caused by common saprotrophs found in the soil and on thorny shrubs in semi-desert climates.[10] Some common causative agents are:[11]
- Madurella mycetomatis (fungus)
- Nocardia brasiliensis (bacteria)
- Actinomadure madura (bacteria)
- Streptomyces somaliensis (bacteria)
- Actinomadura pelletieri (bacteria)[3]
Infection is caused as a result of localized skin trauma, such as stepping on a needle or wood splinter, or through a pre-existing wound.[10]
The first visible symptom of mycetoma is a typically painless swelling beneath the skin; over several years, this will grow to a nodule (lump).[9] Affected people will experience massive swelling and hardening of the area, in addition to skin rupture and the formation of sinus tracts that discharge pus and grains filled with organisms.[9] In many instances, the underlying bone is affected.[12][10] Some people with mycetoma will not experience pain or discomfort, while others will report itching and/or pain.[9]
Diagnosis
There are currently no rapid diagnostic tools for mycetoma.[3] Mycetoma is diagnosed through microscopic examination of the grains in the nodule and by analysis of cultures.[10] Since the bacterial form and the fungal form of mycetoma infection of the foot share similar clinical and radiological features, diagnosis can be a challenge.[2] Magnetic resonance imaging is a very valuable diagnostic tool. However, its results should be closely correlated with the clinical, laboratory and pathological findings.[12][13]
Treatment
While treatment will vary depending on the cause of the condition, it may include antibiotics or antifungal medication.[9] Actinomycetoma, the bacterial form, can be cured with antibiotics.[2] Eumycetoma, the fungal form, is treated with antifungals.[13] Surgery in the form of bone resection may be necessary in late presenting cases or to enhance the effects of medical treatment.[12] In the more extensive cases amputation is another surgical treatment option.[14][10] For both forms, extended treatment is necessary.[2]
Epidemiology
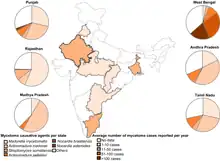
Mycetoma is endemic in some regions of the tropics and subtropics.[1] India, Sub-Saharan Africa as Sudan, and Mexico are most affected.[1][15] Pakistan is probably a moderate-endemic country.[8] Sporadic cases have been reported across some North African countries.[16] Egypt is probably a low-endemic country.[5]
Other animals
In cats, mycetoma can be treated with complete surgical removal. Antifungal drugs are rarely effective.[17]
References
- Zijlstra, Eduard E.; Sande, Wendy W. J. van de; Welsh, Oliverio; Mahgoub, El Sheikh; Goodfellow, Michael; Fahal, Ahmed H. (1 January 2016). "Mycetoma: a unique neglected tropical disease". The Lancet Infectious Diseases. 16 (1): 100–112. doi:10.1016/S1473-3099(15)00359-X. ISSN 1473-3099. PMID 26738840.
- Welsh O, Al-Abdely HM, Salinas-Carmona MC, Fahal AH (October 2014). "Mycetoma medical therapy". PLOS Neglected Tropical Diseases. 8 (10): e3218. doi:10.1371/journal.pntd.0003218. PMC 4199551. PMID 25330342.
- van de Sande WW, Maghoub El S, Fahal AH, Goodfellow M, Welsh O, Zijlstra E (March 2014). "The mycetoma knowledge gap: identification of research priorities". PLOS Neglected Tropical Diseases. 8 (3): e2667. doi:10.1371/journal.pntd.0002667. PMC 3967943. PMID 24675533.
- Sande, Wendy W. J. van de (7 November 2013). "Global Burden of Human Mycetoma: A Systematic Review and Meta-analysis". PLOS Neglected Tropical Diseases. 7 (11): e2550. doi:10.1371/journal.pntd.0002550. ISSN 1935-2735. PMC 3820768. PMID 24244780.
- Ahmed, SA; El-Sobky, TA; de Hoog, S; Zaki, SM; Taha, M (9 September 2022). "A scoping review of mycetoma profile in Egypt: revisiting the global endemicity map". Transactions of the Royal Society of Tropical Medicine and Hygiene. 117 (1): 1–11. doi:10.1093/trstmh/trac085. PMC 9808524. PMID 36084235.
- Buonfrate, D; Gobbi, F; Angheben, A; Marocco, S; Farina, C; Van Den Ende, J; Bisoffi, Z (2014). "Autochthonous cases of mycetoma in Europe: report of two cases and review of literature". PLOS ONE. 9 (6): e100590. Bibcode:2014PLoSO...9j0590B. doi:10.1371/journal.pone.0100590. PMC 4070928. PMID 24963778.
- Barış, Ayşe; Öncül, Ahsen; Öztürk, Kahraman; Barış, Alican; Aykut, Serkan; Aktaş, Elif (19 April 2021). "Mikolojik Tanının Önemi: 20 Yıl İhmal Edilen Bir Scedosporium apiospermum Kompleks Miçetoma Olgusu". Mikrobiyoloji Bulteni. 55 (2): 256–264. doi:10.5578/mb.20219911. PMID 33882656. S2CID 241887330.
- Zeeshan, Mohammad; Fatima, Saira; Farooqi, Joveria; Jabeen, Kauser; Ahmed, Arsalan; Haq, Afreen; Arif, Muhammad Omer; Zafar, Afia (29 July 2022). "Reporting of mycetoma cases from skin and soft tissue biopsies over a period of ten years: A single center report and literature review from Pakistan". PLOS Neglected Tropical Diseases. 16 (7): e0010607. doi:10.1371/journal.pntd.0010607. PMC 9365187. PMID 35905141.
- "Mycetoma". Genetic and Rare Diseases Information Center (GARD). National Institutes of Health. Retrieved 2018-04-17.
- RESERVED, INSERM US14 -- ALL RIGHTS. "Orphanet: Mycetoma". www.orpha.net. Retrieved 2018-04-17.
- Verma, P.; Jha, A. (March 2019). "Mycetoma: reviewing a neglected disease". Clinical and Experimental Dermatology. 44 (2): 123–129. doi:10.1111/ced.13642. PMID 29808607. S2CID 44123860.
- El-Sobky, TA; Haleem, JF; Samir, S (2015). "Eumycetoma Osteomyelitis of the Calcaneus in a Child: A Radiologic-Pathologic Correlation following Total Calcanectomy". Case Reports in Pathology. 2015: 129020. doi:10.1155/2015/129020. PMC 4592886. PMID 26483983.
- Karrakchou, B; Boubnane, I; Senouci, K; Hassam, B (10 January 2020). "Madurella mycetomatis infection of the foot: a case report of a neglected tropical disease in a non-endemic region". BMC Dermatology. 20 (1): 1. doi:10.1186/s12895-019-0097-1. PMC 6953183. PMID 31918687.
- Efared, Boubacar; Tahiri, Layla; Boubacar, Marou Soumana; Atsam-Ebang, Gabrielle; Hammas, Nawal; Hinde, El Fatemi; Chbani, Laila (December 2017). "Mycetoma in a non-endemic area: a diagnostic challenge". BMC Clinical Pathology. 17 (1): 1. doi:10.1186/s12907-017-0040-5. ISSN 1472-6890. PMC 5288886. PMID 28167862.
- Oladele, RO; Ly, F; Sow, D; Akinkugbe, AO; Ocansey, BK; Fahal, AH; van de Sande, WWJ (14 April 2021). "Mycetoma in West Africa". Transactions of the Royal Society of Tropical Medicine and Hygiene. 115 (4): 328–336. doi:10.1093/trstmh/trab032. PMID 33728466.
- Elgallali, N; El Euch, D; Cheikhrouhou, R; Belhadj, S; Chelly, I; Chaker, E; Ben Osman, A (June 2010). "[Mycetoma in Tunisia: a 15-case series]". Médecine Tropicale. 70 (3): 269–73. PMID 20734597.
- Eldredge, Debra M.; Carlson, Delbert G.; Carlson, Liisa D.; Giffin, James M. (2008). Cat Owner's Home Veterinary Handbook. Howell Book House. p. 160.
External links
- DermNet NZ: an online resource about skin diseases from the New Zealand Dermatological Society Incorporated.
- Orphanet: a reference portal from Europe that provides information on rare diseases and orphan drugs.
- ClinicalTrials.gov: a list of clinical trials related to mycetoma.